When diet and exercise stop working, most people assume they’re not trying hard enough. Cut more calories, add more cardio, push harder.
But what if the problem isn’t effort at all?
Research points to cortisol — your body’s stress hormone — as a common culprit behind stubborn belly fat. The kind that refuses to budge no matter what you try.
Cortisol belly fat doesn’t play by normal rules. It accumulates around your midsection, feels different to the touch, and sometimes even increases when you’re eating less. Understanding why starts with understanding how stress rewires your metabolism.
Note: This article provides educational information about cortisol and weight management. Everyone’s body responds differently to stress and hormones. If you’re dealing with stubborn weight gain, consult your healthcare provider to rule out underlying conditions.
Here’s What You’ll Learn
- Why cortisol belly fat behaves completely different from regular fat (and why your usual methods fail)
- The science behind stress-weight connection that most people miss
- 7 specific signs your belly fat is cortisol-related, not diet-related
- What causes cortisol levels to spike (some might surprise you)
- Why calorie restriction can actually make cortisol belly worse
- Natural approaches to support healthy cortisol levels
- The cellular connection between stress and stubborn weight
- …and much more!
What Is Cortisol Belly Fat (And Why It Resists Traditional Methods)
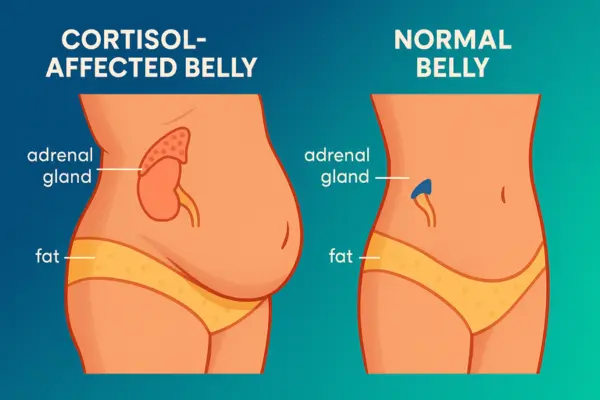
Cortisol is your body’s primary stress hormone. The adrenal glands pump it out whenever stress hits — work deadlines, family drama, even sitting in traffic.
In small doses? Actually helpful. It’s that burst of energy that gets you through tough situations.
The problem starts when stress becomes your default state. Cortisol stays elevated continuously. And elevated cortisol sends a very specific message to your body: store fat.
Not just anywhere. Specifically around your midsection.
Why the belly? Your body doesn’t distinguish between “stressed about bills” and “running from danger.” It just knows stress equals potential threat. Store energy fast, store it where you can access it quickly. That means visceral fat wrapped around your organs.
Here’s what makes cortisol belly different from regular fat.
Regular belly fat distributes more evenly. You can pinch it between your fingers. It responds to calorie deficits like you’d expect.
Cortisol belly fat sits deeper. Feels firmer. Creates that distinct apple shape where your midsection sticks out disproportionately. And it stubbornly resists traditional diet and exercise.
You might lose weight from your face, your arms, your legs. But that belly? Stays put.
The visual difference is pretty obvious once you know what to look for. Cortisol belly tends to protrude more, almost like carrying all your weight in front. People describe it as looking pregnant when they’re definitely not.
This isn’t about vanity. Visceral fat actively produces inflammatory compounds. It’s metabolically different from the soft, pinchable fat elsewhere on your body.
When traditional weight loss methods repeatedly fail, understanding the cellular mechanisms behind stress-related weight gain provides context for why surface-level interventions often miss the mark.
The Cortisol-Belly Fat Connection Science
The relationship between cortisol and belly fat involves a metabolic cascade that most people never learn about.
Stress hits. Your adrenal glands release cortisol. Cortisol signals your liver to dump glucose into your bloodstream for quick energy.
But here’s the thing — you’re not actually running from danger. You’re just stressed. So that glucose just sits there.
Your pancreas notices the excess blood sugar and releases insulin to deal with it. Insulin’s job? Store that energy. And cortisol directs exactly where: your belly.
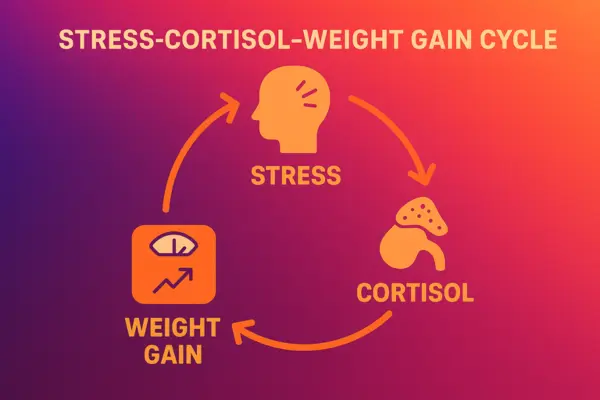
This creates a vicious cycle that feeds on itself.
Chronic stress leads to elevated cortisol. Cortisol triggers visceral fat accumulation. But visceral fat isn’t inert — it actively produces inflammatory compounds. Those compounds? They raise cortisol even more.
Stress, cortisol, belly fat, inflammation, more cortisol, more belly fat. Round and round.
According to research from the National Institutes of Health, chronic stress and elevated cortisol lead to significant increases in abdominal fat, even in people maintaining otherwise healthy lifestyles.
This explains something frustrating. Why calorie restriction often backfires for cortisol-driven weight gain.
When you dramatically cut calories, your body reads this as another stressor. Food scarcity. Times are tough. Better hold onto that belly fat even harder.
The physiological system designed to protect you becomes your enemy. It can’t tell the difference between a real threat and modern life stress.
Important Note: While understanding cortisol’s role helps, persistently high cortisol can indicate serious conditions like Cushing’s syndrome. Rapid weight gain, severe fatigue, or other concerning symptoms warrant medical evaluation and proper testing.
7 Signs Your Belly Fat Is Cortisol-Related
Not all belly fat accumulates for the same reasons. Certain patterns suggest cortisol playing a major role.
The Apple Shape
Your weight concentrates around your midsection while your limbs stay relatively slim. That disproportionate distribution creates an obvious apple silhouette.
Diet-Resistant
You’ve tried everything. Cut carbs, counted calories, increased workouts. Your belly barely budges. Maybe you lose weight from other areas, but not where you want it.
Gaining Without Overeating
Your dietary habits haven’t changed. Maybe they’ve even improved. But your belly keeps expanding anyway. Cortisol triggers fat storage regardless of caloric intake.
Energy Rollercoaster
That brutal afternoon crash around 3 PM. You’d kill for a nap. High cortisol disrupts blood sugar regulation, creating pronounced energy swings throughout the day.
Sleep Problems
You’re exhausted but can’t fall asleep. Or you crash fine but wake at 3 AM with racing thoughts. Cortisol should naturally decline at night — when it doesn’t, quality sleep becomes nearly impossible.
Wired But Tired
Simultaneously exhausted and anxious. Running on fumes but unable to actually rest. Your body stuck in constant high-alert mode.
Firm Texture
Unlike soft, jiggly subcutaneous fat, cortisol belly often feels firmer. Almost bloated. That’s visceral fat surrounding your organs, not the pinchable kind under your skin.
Multiple matching symptoms? Cortisol might be running the show behind your stubborn belly fat.
Recognizing these patterns helps identify when addressing stress and metabolism makes more sense than just eating less. Research into how cellular energy production affects stress response suggests supporting metabolism at a foundational level may help your body handle stress more effectively.
What Causes High Cortisol Levels
Multiple factors keep cortisol elevated. Usually it’s a combination rather than one single cause.
Work Stress
Not occasional stress. The constant low-level anxiety that never really goes away. Emails at 10 PM, impossible deadlines, difficult relationships. Your body doesn’t care if it’s “just work stress.” Stress is stress.
Sleep Deprivation
This one creates a brutal cycle. Stress disrupts sleep, which raises cortisol, which further disrupts sleep. Most people need 7-9 hours but average 6 or less. Each missing hour stacks up.
Diet Issues
Excess refined sugar and carbs spike blood sugar, which triggers cortisol. Too much caffeine keeps cortisol elevated all day. And ironically, severe calorie restriction — the first thing most people try — acts as a major stressor itself.
No Recovery Time
When’s the last time you genuinely relaxed? Not scrolled your phone on the couch. Actually unwound. Most people go from one obligation to the next with zero downtime. Cortisol never gets a chance to come down.
Age
After 35, your body becomes less efficient at regulating cortisol. The same stress you shrugged off in your 20s now hits harder. For women, declining estrogen during perimenopause makes cortisol’s effects even more pronounced.
Hidden Stressors
Chronic inflammation. Digestive problems. Environmental toxins. Relationship tension you’re not actively thinking about. All of these operate in the background, keeping cortisol partially elevated even when you don’t feel consciously stressed.
You probably can’t eliminate every stressor. Life is stressful. But understanding what’s driving your cortisol up helps you figure out where to focus.
Why Traditional Weight Loss Fails for Cortisol Belly
Most people follow the same playbook when they want to lose belly fat.
Cut calories significantly. Do more cardio. Eliminate entire food groups. Exercise harder and longer.
Logical, right? Burn more, eat less, lose weight.
Except when cortisol is the problem, this approach often makes things worse.
Calorie Restriction as Stress
Dramatically cutting calories triggers your body’s scarcity response. Food is scarce, times are tough, better hold onto every calorie. That scarcity signal? Releases more cortisol. Which signals more fat storage, especially around your middle.
Too Much Cardio
Long cardio sessions spike cortisol. An hour on the treadmill when you’re already stressed just adds more physical stress. Some cardio is fine. But chronic cardio when cortisol’s already high? You’re digging the hole deeper.
Extreme Restriction
Keto, paleo, whole30, whatever strict diet you choose adds stress. Mental energy planning meals, saying no to foods, fighting cravings. All of that registers as stress. More cortisol.
The Yo-Yo Trap
Restrict hard. Lose a little weight (probably water and muscle). Feel deprived. Eventually break. Gain it all back plus some. Each cycle makes your body more resistant to weight loss as cortisol regulation gets increasingly dysregulated.
The harder you push with traditional methods, the worse cortisol belly often gets.
Your effort and willpower aren’t the problem. You’re just fighting the wrong battle.
Note: Diet and exercise absolutely matter for overall health. But when cortisol is chronically elevated, addressing the stress response becomes necessary before other interventions can work effectively.
Understanding this counterintuitive relationship clarifies why dedication alone doesn’t always produce results. Exploring how metabolism functions at a cellular level reveals why addressing stress response and metabolic efficiency may provide a better foundation than calorie restriction alone.
How to Lower Cortisol Naturally

When cortisol drives belly fat, addressing stress becomes as important as diet and exercise.
Several approaches show promise for supporting healthy cortisol levels.
Sleep First
Quality sleep is probably the most powerful cortisol regulator. Aim for 7-9 hours in a cool, dark room. Go to bed at the same time each night. Your body regulates cortisol during sleep — skip it, and you’re fighting uphill.
Stress Management
Not “just relax” advice. Practical approaches that actually work.
Deep breathing for 5-10 minutes daily. Sounds simple, but it literally signals your nervous system to shift out of stress mode.
Morning sunlight exposure helps regulate your natural cortisol rhythm.
Setting boundaries around work and personal time. Actually saying no to things that drain you.
Brief periods of genuine quiet. No phone, no TV, no stimulation.
Nutrition for Balance
Instead of dramatic restriction, focus on stability.
Include protein with each meal to balance blood sugar. Moderate refined sugars and carbs rather than eliminating them entirely. Limit caffeine to morning only. Stay hydrated — dehydration itself acts as a stressor. Don’t skip meals, which creates additional stress signals.
Movement That Doesn’t Stress
Exercise helps, but type matters when cortisol’s elevated.
Walking provides benefits without excessive stress. Gentle yoga or stretching activates your parasympathetic nervous system. Moderate strength training 2-3 times weekly builds muscle without prolonged cortisol spikes. Choose activities that feel restorative, not punishing.
Recovery Time
Your body needs time to bring cortisol down between stressors.
Schedule genuine rest days from structured exercise. Allow time for non-productive activity. Engage in things that actually relax you, not just distract you.
Cellular Support
Emerging research suggests efficient cellular function helps your body handle stress better. Supporting mitochondrial function — those microscopic power plants in your cells — may help your system manage cortisol and use energy more effectively instead of storing it as visceral fat.
Foods That Fight Cortisol Belly Fat
No single food eliminates cortisol belly fat. But certain choices may help support healthy cortisol levels while others contribute to elevation.
Foods That May Help
Dark leafy greens like spinach, kale, and Swiss chard pack magnesium, which plays a role in cortisol regulation.
Fatty fish — salmon, sardines, mackerel — provide omega-3s that support stress response systems.
Berries contain antioxidants that may help combat stress-related inflammation.
Avocados deliver healthy fats that maintain stable blood sugar.
Dark chocolate (70% cacao or higher) contains compounds that some research suggests help moderate stress response.
Green tea provides L-theanine, promoting calm alertness without sedation.
Fermented foods like yogurt, kefir, and sauerkraut support gut health, which influences hormone regulation.
Foods That May Elevate Cortisol
Excess refined sugar and carbs create rapid blood sugar swings that trigger cortisol release.
High caffeine intake — more than 2-3 cups daily — can keep cortisol elevated throughout the day.
Alcohol disrupts sleep quality and interferes with cortisol regulation.
Heavily processed foods may contribute to inflammation that compounds stress response.
Timing Matters
Starting your day with breakfast helps establish healthy cortisol rhythm. Eating your final meal 2-3 hours before bedtime allows proper digestion before sleep.
Avoid barely eating all day then having a huge dinner. That pattern creates blood sugar and cortisol chaos.
Hydration
Dehydration represents a physical stressor that elevates cortisol. Aim for 8-10 cups of water daily. Your body can’t regulate hormones efficiently when dehydrated.
These approaches focus on providing resources for healthy stress response rather than creating additional stress through restriction.
The Cellular Connection You’re Missing
Chronic stress affects more than hormone levels. It impacts how your cells produce energy.
Your cells contain tiny structures called mitochondria. Think of them as microscopic power plants converting food and oxygen into usable energy.
When cortisol stays elevated from chronic stress, several changes happen.
Mitochondrial efficiency drops. Cellular energy production declines. Your overall metabolism slows. The body shifts toward energy conservation instead of expenditure.
This explains persistent fatigue even with adequate sleep. When cellular power plants operate inefficiently, you experience genuine energy deficits at a fundamental level.
The connection to belly fat becomes clearer. When cells can’t produce energy efficiently, your body stores more incoming calories as fat rather than burning them for fuel.
Like a furnace running at low capacity. Instead of burning fuel, it just accumulates unused material.
Research indicates supporting mitochondrial function may help your body manage stress more effectively and utilize energy more efficiently.
Rather than forcing metabolism to accelerate, this approach focuses on providing cellular structures with resources needed for optimal function.
This cellular approach to metabolism and stress response represents a different perspective from traditional calorie-focused strategies, addressing function at a more foundational level.
FAQ — Cortisol Belly Fat Questions
Can cortisol belly fat go away?
Yes, but it requires addressing elevated cortisol, not just cutting calories. When cortisol levels normalize through improved sleep, stress management, and metabolic support, your body can gradually release stubborn abdominal fat.
The process typically takes longer than conventional fat loss. Patience and consistency matter here.
How long does it take to reduce cortisol belly?
Timeline varies widely based on initial cortisol elevation and intervention consistency.
Some people notice improvements in energy and bloating within 2-3 weeks. Visible fat reduction usually requires 2-3 months of sustained effort.
It proceeds slower than most people prefer. But this reflects the time needed to reverse patterns that developed gradually over months or years.
Does exercise help with cortisol belly fat?
Exercise type matters significantly.
Gentle movement like walking, yoga, and moderate strength training may help lower cortisol. But intense cardio or excessive training can raise cortisol further.
When stress levels are already elevated, adding more physical stress often backfires. Focus on movement that feels restorative rather than depleting.
What’s the difference between cortisol belly and menopause belly?
These conditions frequently overlap, particularly for women over 40.
Declining estrogen during menopause increases cortisol sensitivity, making stress-related belly fat more pronounced. Many women experience both simultaneously.
Approaches that support healthy cortisol levels may help address both, as they share common hormonal mechanisms.
Can supplements help with cortisol belly?
Some supplements show potential for supporting healthy cortisol levels. Ashwagandha, magnesium, and omega-3 fatty acids have research backing.
But supplements work most effectively as part of a comprehensive strategy that includes sleep optimization, stress management, and nutrition. No supplement alone resolves cortisol issues without addressing underlying lifestyle factors.
Is cortisol belly the same as visceral fat?
Essentially, yes.
Elevated cortisol preferentially stores fat as visceral fat — the type surrounding internal organs. This differs from subcutaneous fat under your skin.
Visceral fat poses greater health risks because it’s metabolically active and produces inflammatory compounds. Addressing cortisol belly serves health purposes beyond appearance.
Why does stress cause belly fat specifically?
From an evolutionary perspective, your body stores fat in the abdominal region during stress because this location allows quickest energy access for fight-or-flight responses.
The physiological system doesn’t distinguish between modern stressors like financial worry and physical threats. It responds to stress signals by storing readily accessible energy in your midsection.
Can you have high cortisol without feeling stressed?
Absolutely.
Mental perception of stress doesn’t always match physiological stress levels. Physical stressors like poor sleep, blood sugar imbalances, chronic inflammation, or digestive issues can keep cortisol elevated without conscious stress awareness.
Additionally, people sometimes adapt to chronic stress as their normal state, losing awareness of their elevated stress baseline.
For those who’ve struggled with stubborn midsection weight despite dedicated efforts, learning about comprehensive approaches to metabolism and cellular function may provide additional perspective on addressing weight challenges from multiple angles.
The Bottom Line on Cortisol Belly Fat
Stubborn belly fat that resists traditional approaches may signal elevated cortisol rather than insufficient willpower.
Cortisol belly fat differs physiologically from regular fat. It requires strategies addressing the root cause — chronic stress and hormonal dysregulation — rather than simply reducing calories or increasing exercise intensity.
Your body naturally releases stored visceral fat when given appropriate conditions.
Adequate, consistent sleep. Effective stress management. Balanced nutrition without severe restriction. Movement that supports rather than stresses your system. Cellular support for efficient metabolic function.
This process doesn’t produce rapid transformation. Sustainable results take time as your body gradually rebalances hormonal patterns and metabolic function.
But this approach addresses underlying causes instead of just managing symptoms.
For those dealing with belly fat unresponsive to conventional methods, investigating deeper metabolic factors may prove valuable.
The issue might not be insufficient effort but rather incomplete understanding of what’s actually happening beneath the surface.
Sometimes effective solutions come not from working harder at unsuccessful strategies, but from working smarter by understanding and addressing root causes.
Note: If you found this information helpful and want to explore how cellular metabolism relates to stress response and weight management, detailed information about one approach to mitochondrial support may provide additional context for understanding metabolic function at a foundational level.
Important Medical Disclaimer
This article is exclusively informational and educational. It is not intended to diagnose, treat, cure, or prevent diseases.
Always consult a qualified healthcare professional before starting any type of supplementation — especially if you are pregnant, breastfeeding, taking continuous-use medications, or have any pre-existing health conditions. Learn more here
Transparency and Affiliate Disclosure
This article may contain affiliate links. This means that when you make a purchase through one of these links, we may receive a commission — at no extra cost to you.
This commission helps us keep the rootssprout.com blog running, publishing free, honest content based on reliable information.
We only recommend products that we research thoroughly, evaluate with editorial responsibility, and believe can truly help our readers.
To better understand how affiliate links work and our commitment to transparency, visit our complete disclosure page: Transparency and Affiliate Disclosure